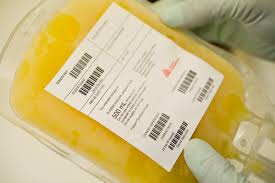
Recently, we received word of a voluntary recall of a particular brand of immune globulin (IG). The manufacturer requested pharmacies to return all units of two specific lot numbers of the product because of reports of allergic-type reactions in patients who had been infused with these specific lots.
The hives, swelling, and skin redness that patients experienced quickly resolved when they were treated with antihistamines (Benadryl, for example), steroids, and Tylenol. Still, the manufacturer wanted to be sure others were not unduly affected by these uncomfortable symptoms caused by their intravenous IG infusions.
While news of a recall may alarm some patients, making them question the safety of their therapy, veteran IG users know that the rare recall of medications is usually not a cause for concern. In fact, the idea that the manufacturer is vigilant enough about their products to take this step voluntarily makes them feel more confident in their treatments.
Product recall or withdrawal is a common practice in industries across the country, including pharmaceuticals and medical devices. A product recall or withdrawal has several different levels; the highest is a Patient Level Recall, which is a request or warning to stop using a product. This directive can come from the Food and Drug Administration (FDA), which oversees drug safety. More often, however, the request comes voluntarily from the manufacturer, usually in response to some safety concern they’ve noticed.
“We get recall notices from both the FDA and manufacturers,” says Jack Lemley, Pharm.D., Chief Pharmacy Officer at CSI Pharmacy. “Any time we receive a recall alert, we review our electronic inventory to determine if we have ever purchased the affected lot numbers. If we have, we then check to see if any of it is still in stock and remove it.”
Still, there are times when a recalled product may be dispensed before pharmacists are aware of the recall. At CSI Pharmacy, if such a product has been shipped to a patient, pharmacists contact the person immediately and advise not to infuse the therapy, if appropriate to the level of the recall. If the patient has already infused the product, pharmacists will evaluate them for any adverse reactions. Patients are urged to notify their healthcare provider(s) of any potential adverse effects for their IG therapy, even if there is no known recall.
As a partner in their own healthcare, we strongly encourage patients to keep their own records. This should include the manufacturer of the product, the lot number (found on the side of the bottle or container), and the way it was administered (IV or subcutaneous). CSI Pharmacy provides patients with an infusion log used to record this information.
Patients can be proactive in finding out about IG product “events,” as recalls and withdrawals are called, by registering for the Patient Notification System (PNS). Through this free, confidential early warning system, patients can be made aware of a recall before they infuse or inject their therapy.
The PNS was developed by producers and distributors of plasma products and is led by the Plasma Protein Therapeutics Association (PPTA) in response to consumer requests. It provides registrants with automatic updates about plasma product withdrawals and recalls from all participating manufacturers.
To access the Patient Notification System, call 1-888-UPDATE-U (1-888-873-2838) or register online at www.patientnotificationsystem.org. You can choose the products with which you would like to receive notifications, as well as the method of notification: via telephone, fax, e-mail, or overnight letter. You will also receive a first-class letter by the US Postal Service when there are notifications.
While pharmacists do everything possible to ensure the safety of patients, there’s always a chance that a product may slip through. The Patient Notification System in one more way you can team up with your pharmacists to ensure your health and peace of mind.